The Cost of Providing Care
Caring for someone with Alzheimer’s or other forms of dementia can be physically, mentally and financially taxing. In fact, a 2019 Genworth study found that the median cost of in-home care in the US is close to $52,000 per year. And nursing home care? A whopping $102,200 per year.¹
Caregiving is big business, but much of it comes pro bono as family and friends tend to take on the responsibility themselves in lieu of professional help.

The hidden costs of caregiving exist in multiple forms.
- Many caregivers are still in the workforce and face lost wages due to time off while caregiving or dropping out of the workforce entirely.
- The cost of gas or other transportation expenses can add up while chaperoning loved ones to doctors appointments and other engagements.
If the person receiving care does not have adequate insurance, income or savings, caregivers can end up holding the tab for additional costs such as:
- Fees for respite care, adult day care services, nursing homes and assisted living centers.
- Prescription medication and at-home medical equipment such as walkers and monitors.
- Out-of-pocket costs for doctor’s appointments and hospital visits.
Adding to the cost of care is the fact that our average age of death has increased from 69.7 in 1960 to nearly 79 today.2 People living longer means people needing care longer. And the more effective you are at caring for someone, the longer they may need treatment.
Considering the cost of Alzheimer’s care, it’s no mystery why so many people opt to take on caregiving alone rather than summoning professional help. According to the Alzheimer’s Association, Alzheimer’s recently became the most expensive condition in the country to treat, with annual costs of care exceeding $214 billion.3 And with annual worldwide costs exceeding $600 billion, dementia care would be the world’s 18th-largest economy if it were its own country.4
Given the cost responsibilities of care, what’s a caregiver to do?
How Medicare Helps
The financial blow of caregiving can be partially absorbed if the person receiving care has Medicare insurance. There is no simple answer to the question of whether or not Medicare covers Alzheimer’s. Original Medicare does not exactly cover Alzheimer’s itself but it does provide coverage for many of the services required of an Alzheimer’s patient.

Some of the services that are at least partially covered by Original Medicare (Part A and B) or Medicare Advantage plans that may be utilized by a person with Alzheimer’s include:
At-home skilled nursing care
Intermittent skilled nursing care may be covered by Part A of Medicare if the person is under the care of a doctor and is certified as homebound. People with late-stage Alzheimer’s may be deemed homebound because they may be psychologically unfit to leave their home.
Therapy
Occupational therapy is covered by Part B when deemed medically reasonable and necessary. Annual cap limits apply.
Durable medical equipment
While generally not directly related to dementia, many people suffering from the condition require the use of walkers, wheelchairs and other equipment that may be covered by Part B as “durable medical equipment.”
Hospice care
Part A of Medicare provides coverage for hospice care. The Alzheimer’s Association reports that the use of hospice care among Alzheimer’s patients is on the rise, with a 28 percent increase from 2000 to 2009.5
Respite care
If a caregiver needs some time off from their duties, Part A of Medicare provides coverage for inpatient respite care.
Clinical research
Both Part A and Part B of Medicare cover certain clinical research studies that may involve the testing of medications and other treatments for dementia.
Diagnostic testing
Medicare Part B will cover the cost of diagnostic testing including CT scans, PET scans and MRIs if requested by a physician. Such scans can help detect changes in brain cognition that may signal a presence of Alzheimer’s.
Cognitive assessment
Medicare Part B also provides coverage for a cognitive assessment during an annual wellness visit to help detect any signs of mental impairment.
Mental health care
Alzheimer’s disease is often accompanied by feelings of depression, anxiety and other psychological or psychiatric problems. Part B of Medicare covers outpatient visits with mental health professionals that can include depression screenings, psychiatric evaluations and even family counseling. Part A provides coverage for inpatient stays at mental health facilities.
Medicare Part D and Medigap
Medicare Part D provides coverage for prescription medication and certain Part D plans may cover some of the medications used to treat dementia. Medication may be used to treat a condition that’s causing dementia, to maintain mental functioning, prevent further strokes in people who have vascular dementia or to treat some of the mood and behavior problems associated with dementia. According to Consumer Reports, the average Alzheimer’s patient pays around $177 per month for their medications with that number sometimes reaching as high as $400 per month.6 Fortunately, most standard Alzheimer’s medications are on Medicare’s list of approved drugs.
Medigap, or Medicare Supplement Insurance, provides coverage for some of the out-of-pocket expenses that may be incurred by Original Medicare. These include deductibles, copayments and coinsurance.
Additional Financial Assistance
Although it isn’t easy for family caregivers to receive compensation for their hard work, that doesn’t mean caregivers and their loved ones aren’t without options for financial resources.

Long-term care insurance
If a person is enrolled in long-term care insurance prior to being diagnosed with Alzheimer’s, they may be eligible to receive a daily benefit payout that can be used for caregiving expenses.
Disability insurance
A person who enrolls in disability insurance prior to receiving an Alzheimer’s diagnosis can collect the amount of money tied to the policy as a way to help pay for care. For personal policies, the benefits received will be the amount the person chose when the policy was activated. For employer-paid policies, the amount is often 60-70 percent of the person’s gross income.
Life insurance
Some life insurance policies offer accelerated death benefits, meaning cash from the policy can be paid out in the event of a terminal illness such as Alzheimer’s. Other life insurance policies may be borrowed from, and the funds can be used to assist with caregiving expenses.
Supplemental Security Income
Supplemental Security Income (SSI) provides a monthly benefit for people age 65 and over who are disabled, have limited income and assets and meet the Social Security Administration’s definition of disability.
Medicaid
Medicaid provides medical coverage and long-term care for people with low income or who have exhausted their own money paying for care. While eligibility and benefits vary from state to state, a person with dementia who qualifies for Supplemental Security Income will usually qualify for Medicaid.
Many states have both Medicaid and non-Medicaid programs available that while not specifically designed for people with Alzheimer’s, many people with Alzheimer’s will qualify based on their income and need for assistance. An extensive list of these state-specific programs can be found here.
The Family and Medical Leave Act
While federal law cannot help caregivers recoup lost wages, it can offer some job security. The Family and Medical Leave Act (FMLA) provides up to 12 weeks of unpaid leave every year for employees in every state to care for a sick spouse, parent or child without losing their job or forfeiting their health insurance. The law applies only to companies with 50 or more employees and the employee must have worked at least 52 full-time days or 1,250 hours in the previous year to qualify.
Alternative Medicine and Therapies
Traditional medicine isn’t the only way dementia may be treated. Approximately one third of U.S. adults use some form of alternative medicine7 and many of those are using such forms of medicine to treat Alzheimer’s and other types of dementia. Some of the alternative treatments thought to aid in the treatment of Alzheimer’s include:
- Caprylic acid and coconut oil
- Coenzyme Q10
- Coral calcium
- Ginkgo biloba
- Huperzine A
- Omega-3 fatty acids
- Phosphatidylserine
- Tramiprosate
While the effectiveness of these treatments can be debated, one thing is for certain: they cost caregivers and their loved ones money. Health insurers are allowed to limit coverage for things they deem experimental or not medically necessary and as a result, alternative medicine is not often covered by insurance.
That doesn’t mean caregivers aren’t without options though. Some things caregivers can do to try to alleviate the cost of alternative medicines include:
- Calling their loved one’s insurance company
Some insurance companies may provide coverage for an alternative form of medicine if it’s supported by an adequate amount of evidence regarding safety and/or effectiveness. Or they may cover it if there is a referral from a practitioner. It never hurts to call the insurance company and discuss the type of treatment and the coverage options.
- Contacting alternative medicine providers
If the existing insurance policy does not provide coverage for alternative medicine, it may be helpful to contact the provider of the alternative medicine to see which (if any) insurance companies they work with.
- Negotiating
Many people may not realize it, but medical costs are sometimes negotiable. The provider of an alternative medicine may be willing to accept a payment plan or negotiate a discount for bulk purchases.
For Alzheimer’s caregivers looking for more affordable options to help their loved one, a number of alternative therapies exist that offer a way to treat Alzheimer’s in a way that can sometimes be more affordable than traditional medicine.
Aromatherapy
Aromatherapy, or the breathing in of natural oils extracted from flowers, bark, leaves and other parts of plants, has been shown to be an effective way of stimulating brain function in people with Alzheimer’s.8
While research remains young, the benefits of aromatherapy are no less promising. Recent findings have shown lavender and lemon balm to reduce anxiety and agitation, peppermint can stimulate memory and boost appetite, bergamot combats depression and improves mood while rosemary helps with both memory and cognition.
Perhaps the biggest benefit of aromatherapy is the price. These oils can be found in many of the bath soaps, body oils and lotions found at the local supermarket.

Music
Studies have shown that listening to classic hits and show tunes have allowed people with Alzheimer’s to better recall memories and emotions.9 Researchers point to several reasons why music may be helpful in combating Alzheimer’s, including how music evokes emotions and memories, how musical aptitude is among the last remaining abilities in Alzheimer’s patients, and how music can affect mood, help manage stress and stimulate positive interactions.
Alzheimer’s patients have been known to remember musical lyrics long after forgetting familiar faces and names. Neurologic research suggests connections between music and activity in particular parts of the brain that are responsible for creativity, pleasure, emotions and more.
Music therapy is an easy and affordable way for caretakers to help their loved ones with Alzheimer’s. Many older adults still have old records or tapes around the house and CD’s of older music can often be purchased online for a minimal cost. And of course, a caretaker can always just tune a radio to an oldies station.
Gardening
Gardening has several advantages for people battling Alzheimer’s. Any amount of exercise — even just the small movements required of gardening — can be beneficial to people with Alzheimer’s. Gardening can also foster a sense of accomplishment and boost confidence while creating a sense of community and purpose.
It’s not just the act of gardening that can be beneficial either. The garden itself provides a peaceful and relaxing environment for people with Alzheimer’s to spend some time. The fresh air and bright colors of a garden can stimulate the senses, promote brain activity and ward off emotions like anxiety and depression. A garden can also serve as a place of socialization to counter the sense of loneliness that so many people with Alzheimer’s experience.
Scientific studies have shown horticultural therapy to be effective in improving the functional levels of people with Alzheimer’s.10 And of course, gardening helps improve the quality of life for a person with Alzheimer’s in a way that is easy and inexpensive.
Puzzles and games
It’s often discussed that various puzzles and games can help ward off dementia by keeping the brain active and healthy. But what about people who have already been diagnosed with Alzheimer’s?
It turns out that the progression of Alzheimer’s can be slowed even after diagnosis by engaging in crossword puzzles, jigsaw puzzles, word searches and other games that require cognitive thinking. In fact, it’s estimated that regular engagement can lead to a 6-9 month delay in the progression of the disease.11 Such games can keep the neural connections in one’s brain active and strong and improve mental agility. The phenomenon of engaging one’s mind in this type of mental stimulation points to the adage of “use it or lose it.”
Puzzles and games are cheap and easy to come by. If there aren’t any around the house, they can often be found at thrift stores and yard sales.
Video games
Tests have shown that video games can help improve reaction time, memory, the ability to multitask and overall cognitive function.12 In fact, many nursing homes around the country have installed video game consoles for residents to enjoy.
The evidence of these benefits is so strong that some video game companies have begun to develop games that are specifically designed for people with dementia. There’s even hope that video games may one day replace pills in the treatment of cognitive diseases such as Alzheimer’s.
Caretakers needn’t fork over hundreds of dollars for the latest video gaming system, however. There are a number of free or low-cost games available for download on smartphones, tablets and computers that can be enjoyed by people with Alzheimer’s.
Massage
Massage therapy can help ease the effects of isolation and loneliness, increase body awareness and alertness and reduce feelings of confusion or anxiety. One study found that just a five-minute hand massage was effective in decreasing the frequency and intensity of agitated behavior found in people suffering from Alzheimer’s.13
People suffering from Alzheimer’s may have a hard time connecting with another human on an emotional level. But even though they may be void of certain mental abilities, Alzheimer’s does not rob people of their ability to feel physical touch. Massage is a great way for caretakers to connect with their loved ones and express their love in a way that may be easier to understand. Plus, massage improves blood flow and circulation and releases endorphins, all things that can help stimulate the brain.
Caretakers don’t need to hire a professional massage therapist either. Basic massage techniques can be easily learned from resources like YouTube.
Flashing light therapy
A recent study conducted at MIT found that flashing light therapy may be able to reduce the risk of toxic beta amyloid proteins in the brain.14 The buildup of these proteins on the brain clump together to form a sticky plaque that is thought to contribute to the cognitive decline brought on by Alzheimer’s. Drugs have been mostly ineffective at reducing the buildup of these proteins but the scientists at MIT may have discovered a different and more promising approach.
Flashing light therapy involves the use of lights that flash at various speeds and levels of brightness. This visual stimulation helps brain neurons operate at higher levels of gamma frequencies.
Flashing light therapy is still in the early stages of research as an alternative method of Alzheimer’s treatment, but given the minimal investment, it’s worth a shot for any caretaker looking for a more affordable treatment option for their loved one. While light therapy boxes cost into the hundreds of dollars, they can actually just be made at home.
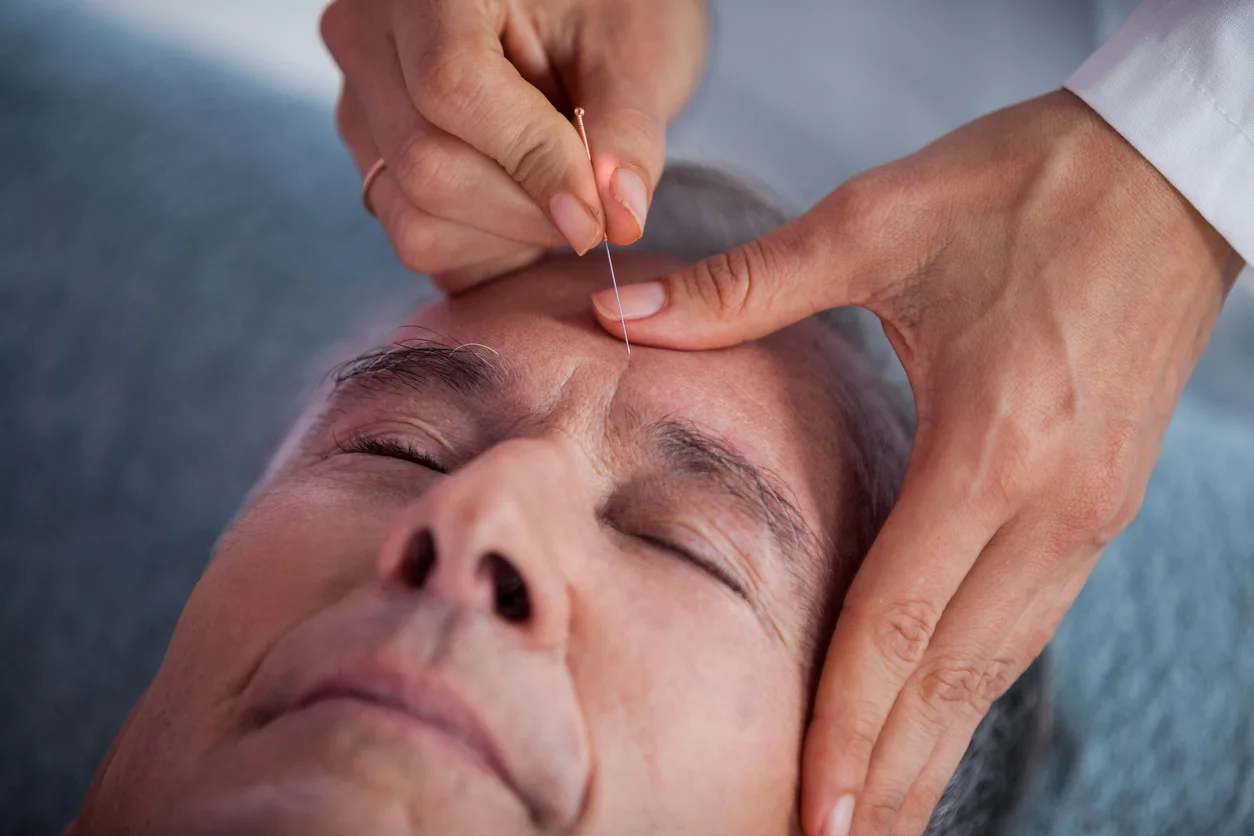
Acupuncture
Acupuncture has long been used to treat a wide range of ailments, including Alzheimer’s. Studies have shown that the practice can be effective in increasing verbal and motor skills along with improving mood and cognitive function in people with Alzheimer’s.15
The ancient Chinese practice of acupuncture is based on the theory of Qi, or patterns of energy that flow through the body and cause disease when these patterns are interrupted. Acupuncture reroutes this energy to restore normal functioning in the body.
While it may sound difficult to believe, acupuncture is actually recognized by the Food and Drug Administration and is widely practiced throughout the U.S.
It is not recommended for caregivers to administer acupuncture themselves, as this practice should be performed only by a professional. But coupons, groupons and discounts for acupuncture are readily available. Acufinder is a searchable database of over 30,000 acupuncturists located all over the U.S. that caretakers may use to find one near them.
Diet
“Brain food” has proved to be quite real when it comes to fighting Alzheimer’s disease. A ketogenic diet, one rich in fat and protein but low in carbohydrates, has been shown to slow and even reverse symptoms of dementia such as memory loss and cognitive impairment.16
A ketogenic diet is high in fish, poultry, eggs, leafy greens and above-ground vegetables, high-fat dairy products like hard cheeses and butter, nuts, seeds and berries. Grains, sugar and fruit are avoided. Basically, the brain of a person with Alzheimer’s can no longer use carbohydrates to produce energy but can still use the molecules found in ketogenic foods to do the same.
A new diet may sound expensive, but caretakers can simply stop buying the foods that do not meet these demands and replace that cost with foods that do.

Exercise
Research has shown that levels of tau, a protein associated with Alzheimer’s, decrease with regular exercise.17 Alzheimer’s patients who regularly exercised have also been found to experience less anxiety, depression and irritability.
Exercise can also help to establish a daily routine, which can be instrumental for people with Alzheimer’s, along with a sense of accomplishment.
The Alzheimer’s Research and Prevention Foundation recommends at least 150 minutes per week of exercise for people with Alzheimer’s.18 The exercise doesn’t have to be anything vigorous, anything from walking, jogging, dancing, swimming or light aerobics can get blood circulating to the brain and stimulate cognitive functioning. And of course, it doesn’t cost anything for a caretaker to take a walk around the block with their loved one.
Pets
Having a pet can help with many of the symptoms of Alzheimer’s disease such as depression, anxiety, loneliness and irritability and help a person become more interactive. It’s no wonder why so many nursing homes have dogs, cats or other pets living there to keep the residents company.
One complex symptom of Alzheimer’s disease is “sundown syndrome,” which is when Alzheimer’s patients experience a great deal of anxiety and aggressive behavior in the evening hours. Researchers at the University of Nebraska Medical Center College of Nursing found that dogs can help Alzheimer’s patients find relief from sundown syndrome.19
Dogs and cats can be rescued from shelters for a nominal fee. And for a caretaker who feels that caring for a pet would add too much extra hassle, they can always just bring their own pet along for visits with their loved one.
FAQ
There’s a lot that caregivers need to know about Medicare. Below are some frequently asked questions that may be helpful to those caring for someone with Alzheimer’s.

- Can a person under 65 get Medicare if they have early onset Alzheimer’s?
Yes. The Social Security Administration recognizes early onset/younger-onset Alzheimer’s as among its Compassionate Allowances initiative. As such, people under the age of 65 who have been diagnosed with early onset Alzheimer’s may receive Social Security Disability Insurance (SSDI) benefits along with Supplemental Security Income (SSI). And if you are under the age of 65 but have been receiving SSDI benefits for at least 24 months, you are eligible for Medicare.
- Will Medicare cover home delivered meals?
Medicare does not provide coverage for home delivered meals. However, there are a number of meal delivery programs that can be utilized by people with Alzheimer’s and their caregivers. Silver Cuisine, Magic Kitchen and Meals on Wheels are all popular options with prepared meals often priced under $10.
- Will Medicare pay for personal care or homemaking services?
Those suffering from the later stages of Alzheimer’s will often need assistance with bathing, dressing, cleaning and other household chores. Medicare does not pay for such services but there are some affordable options available for seniors.
Among the more prominent organizations is the Volunteers of America, which offers home and personal care services to seniors on a volunteer basis.
- Are there any Medicare Special Needs Plans (SNP) that are designed for people with Alzheimer’s?
Yes. Medicare Special Needs Plans (SNP) are insurance plans that are restricted to people with certain characteristics, conditions or diseases. Dementia is one of the qualifying conditions that can make a person eligible for enrollment.
- Does Medicare cover counseling for caregivers and other family members of people with dementia?
Medicare provides coverage for grief and loss counseling for the family members of hospice patients. If a person with Alzheimer’s enters hospice care, their caregiver and other family members may receive such counseling.
Resources for Caregivers
There are a number of resources that can provide caregivers with further assistance.
Family Caregiver Support Program (FCSP)
This federally funded program provides information and assistance to caregivers including counseling and support groups, education and training and even some respite care. The program also allows caregivers to purchase needed supplies such as emergency response systems and home modifications.
Benefits Checkup
The National Council on Aging has an online service dedicated to helping older adults and their families locate and enroll in local, state and federal private benefit programs.
Alzheimer’s Association
The Alzheimer’s Association offers a number of services for caregivers including support groups, caregiver training, legal help and more both online and within local chapters. There’s even an Alzheimer’s caregiving app that can help caregivers coordinate care, manage health information, track medications and access various resources.
Family Caregiver Alliance
Family Caregiver Alliance (FCA) aims to improve the quality of life for caregivers through advocacy, research, education and various services and provides assistance with the development of public and private programs for caregivers.
National Institute on Aging
The National Institute on Aging provides helpful information about caregiving that can be delivered to one’s email and a staff that can direct caregivers to resources available in their local area.
Alzheimer’s Foundation of America
The Alzheimer’s Foundation of America provides caregivers with information including webinars, research studies and support groups along with a toll-free hotline for caregiving help and advice.
TrialMatch
Run by the Alzheimer’s Association, TrialMatch is a way for caregivers to find and enroll in clinical trials related to Alzheimer’s treatments.
Alzheimer’s Prevention Registry
The Alzheimer’s Prevention Registry is a database that connects Alzheimer’s researchers with patients for study participation and offers online classes about the medical, legal and financial aspects of caregiving.
BrightFocus Foundation
The BrightFocus Foundation helps caregivers find professional services, legal and financial assistance, caregiver support programs and more.
*This content is not medical advice, nor is it a substitute for professional medical advice, diagnosis, or treatment.
Sources:
1www.pro.genworth.com/riiproweb/productinfo/pdf/282102.pdf
2data.worldbank.org/indicator/SP.DYN.LE00.IN?locations=US
3health.usnews.com/health-news/health-insurance/articles/2014/10/15/an-alzheimers-complication-some-care-may-not-be-covered-by-medicare
4www.payingforseniorcare.com/alzheimers/financial-assistance.html#title9
5www.alz.org/documents_custom/2016-facts-and-figures.pdf
6www.consumerreports.org/cro/2012/07/evaluating-drugs-to-treat-alzheimer-s-disease/index.htm
7health.usnews.com/health-news/health-insurance/articles/2015/03/09/does-your-health-insurance-cover-alternative-medicine
8www.ncbi.nlm.nih.gov/pubmed/20377818
9www.alzheimers.net/2014-07-21/why-music-boosts-brain-activity-in-dementia-patients/
10www.ahta.org/journal-of-therapeutic-horticulture-18—2007-2008
11www.unforgettable.org/blog/what-are-the-benefits-of-dementia-jigsaw-puzzles/
12www.medicaldaily.com/preventing-alzheimers-disease-video-games-may-help-seniors-retain-cognitive-370690
13www.linkedin.com/pulse/touch-compassion-massage-therapy-alzheimers-disease-van-blaricum/
14www.alzheimers.net/1-25-17-flashing-light-therapy-for-alzheimers/
15www.alzheimers.net/11-19-14-acupuncture-for-alzheimers/
16universityhealthnews.com/daily/memory/ketogenic-diet-shows-promising-results-for-all-dementia-stages/
17www.nbcnews.com/health/aging/better-treatment-alzheimers-exercise-n397461
18alzheimersprevention.org/4-pillars-of-prevention/exercise-and-brain-aerobics/
19www.onecallmedicalalert.com/blog/2013/06/alzheimers-article/









